WRITTEN BY: KATHY FULTON
Mark and I are planners. Me more so, but him too. When we moved to Haiti more than 2 years ago, I wanted a plan in case we had a medical emergency while in our Port au Prince home (the hospital where we work is over an hour’s drive from our home). So last month, when Mark became very ill, we tried what we knew to do at home, but finally realized we needed to implement our back-up medical plan. Mark has a medical condition that flares up from time to time. Sometimes it resolves on its own; sometimes we need to go to the ER. This time he needed the ER. He needed a surgeon to put him under for the short procedure that was required, or the situation could quickly become life-threatening.
So about 5:45pm, I began gathering things for the ER. We had never visited this ER, but had heard that if you live in Port au Prince, this is the one to go to. I wasn’t sure what to bring. Would they have potable water? Would they have food? Did I need to bring our own sheets? Would I have access to electricity to charge my phone, or did I need my external battery charger? Would there be a surgeon on call? Would he/she be familiar with this medical situation? What medical supplies and medicine would I need to bring that they might not have on hand? I understand firsthand the difficulties with providing medical care in a developing country, where certain medicines and supplies are not found in country, and procuring supplies can be a long and complicated process, and where medical facilities are often operating on a shoestring budget. Been there, done that.
I rushed around the house, knowing that I would need to drive, and preferably not in total darkness. When I finally had my bag packed, night was falling. We loaded up and took off into the night as darkness surrounded us. Driving in Port au Prince is difficult (if you want a visual, search “Don’t Drive Here Port au Prince” on YouTube). In the dark, it is more difficult. Although Mark was in great pain and quite nauseated, he tried as best he could to watch for the many approaching vehicles without headlights or lights of any kind, and warned me in case I had not seen them already. I kept my eyes peeled for the throngs of people walking alongside or in the road, and for motorcycles weaving in and out of traffic. Finally, we turned down the road where we knew the hospital was. There was a myriad of people selling their wares on both sides of the road, leaving room for but one vehicle at a time. Smoke from food vendors wafted over the road, casting eerie shadows in the headlights. When oncoming cars approached, the people squeezed into tiny spaces along the road, leaving just enough room for the two vehicles to pass. We saw a facility on our right through an open gate. “I hope that’s not it”, I said under my breath. It was indeed the hospital we were looking for.

Photo Credit: “Night Scene” (Jorge Saenz, AP)
All the medical personnel in the room were indigenous, plus 2 women from Canada, a nurse and a physician, who has just arrived with a team that morning. Although I know there are excellent Haitian nurses and physicians in Haiti, it was somehow comforting to talk with medical professionals I could communicate with completely, in English, who were most likely familiar with the condition Mark has that is rare in Haiti. They told me a surgeon and anesthesiologist were with their group and would be returning shortly. I explained to the Canadians Mark’s condition, and the medicines he would need. The ER there did not have what he needed, but the Canadian ER physician reached into her fanny pack and pulled out one vial of exactly what he needed that she had brought into the country with her that morning. We entered the gates and parked in the area that held about 10 cars – not much parking was necessary as most patients come on foot, motorcycle, or tap-tap. I helped Mark to the doors that said “Salle d’urgence” – Emergency Room. I opened the door to a rectangular room, 15’x30’, with exam tables, cupboards, chairs, and supplies lining the edges to shrink it to about 8’ x 20’. There were about 8-10 patients with varying ailments, and 6-8 medical professionals. No admitting area or desk. When we entered, a nurse looked up and in Haitian creole I said “I think we’re lost. We need the Emergency Room”. They told me I was in the right place.
Payment was required before medical treatment could commense. I took the appropriate forms out the door, around the corner, and down an alley to the cashier office. With the generator humming and people surrounding me talking loudly in the hot, humid night, I could barely hear the cashier’s low voice through the small hole in the glass. I asked the armed guard next to me to help me understand her. Two thousand, five hundred gourdes. Could I pay in US? I asked. Yes, $38. I handed her two $20s. “I don’t have change now; you will have to come back later”. She stamped my paper and I took it back to the ER. Now Mark could get his ER consultation and x-rays he needed.
At this point I saw my world through two sets of eyes. From my American perspective, I saw a whole emergency department crammed into one room, where each person saw every other person’s condition, where bodily fluids, gauze, and other medical disposables were on the floor. I thought of how far we were from sterile, wondered if someone might bump into a nurse giving Mark an injection in the crowded room, and wished I had US standard of care here.
The other set of eyes I looked through were the eyes of someone living in Haiti, where I am aware that most of the people I know could not afford this hospital, even the $40 I paid that night to cover consultation, IVs, pain and nausea medication, and the surgical procedure. This set of eyes was tearfully appreciative that this facility was in existence, as a man who had had a motorcycle accident was being sewn up, as a woman who had a stroke was being cared for, as an elderly man with hypertension was getting the medication he needed to survive, and where my husband would be delivered from a life-threatening situation. How fortunate we were to have access to all of this.
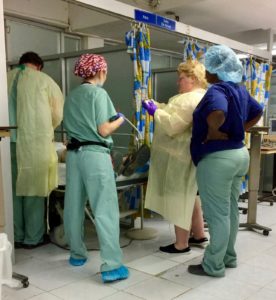 After we waited a couple more hours, the surgeon entered and I expressed my appreciation through tears. They got special permission to use the recovery room to do the procedure rather than do it in the ER room, with the crowd of people there. He brought his anesthesiologist with him. Although the recovery room looked much different than what we would see in the US, I knew Mark was in good hands and that this team understood what my US perspective was as far as quality of care and pain management. They finished the procedure and waited for Mark to awaken. Forty-five minutes later he was released, not because that was ideal, but because there were no more beds available in the hospital.
After we waited a couple more hours, the surgeon entered and I expressed my appreciation through tears. They got special permission to use the recovery room to do the procedure rather than do it in the ER room, with the crowd of people there. He brought his anesthesiologist with him. Although the recovery room looked much different than what we would see in the US, I knew Mark was in good hands and that this team understood what my US perspective was as far as quality of care and pain management. They finished the procedure and waited for Mark to awaken. Forty-five minutes later he was released, not because that was ideal, but because there were no more beds available in the hospital.
I wheeled Mark out to our car, past a few dozen people sleeping on the ground, waiting on their loved ones who were admitted and staying in the open ward. Mark got in the car, and after I went back to the cashier to get paperwork stamped, we were free to go. I maneuvered my way through the night, easier this time since it was after midnight and the streets were fairly clear… until I saw a car stopped in the middle of the road, with police officers nearby. I began to pass, but was flagged down by an officer – one of the many checkpoints we encounter from time to time. I gave him our papers and my Haitian driver’s license. He said something in Creole that I didn’t understand. I asked him to repeat himself. Where is your Passport? Where is your Permis? Most of the police officers we encounter in Haiti are good folks, just doing their job. Once in a while, we encounter one who hassles us to try to get bribe money, or maybe just honestly doesn’t know the law. We explained in detail the papers we had and that they were what was required. When he saw we knew the law, he rolled his eyes and waved us on.
I backed into our space in our neighborhood and helped Mark into our house. A Haitian friend in our neighborhood accompanied us, helping carry our things. He asked how things went. We told him we were so grateful a surgeon was available, but he would be leaving in a few days. We hoped this procedure would get Mark back on his feet. Our friend, who has never been out of Haiti, looked at us with genuine concern and said that maybe we needed to go back to the US to get medical help, because Haiti doesn’t have all that it needs in the world of medicine.
I entered the house and closed the door and fell apart. How blessed I was to have the surgical team! How shocked I was at the condition of the ER! How grateful I was that we can afford the $40 I paid to get the medical care we received! How troubled I was that so many in this country could not afford the same!
…and our friend who helped us in that night. If he were in the same condition, and if he needed medical care beyond what was available in Haiti, he would not have the opportunity to seek care in the US. And yet, knowing that we do have access, he honestly wished for us that we could access the high quality medical care he knew we could receive in our home country. I saw the face of Christ in him that night.
So what do I take from all this? First of all, I am thankful for answered prayers that night, that my husband is alive and well and was well-cared for. Beyond that, I will never make sense of why I have so much privilege, and why so many live without. I just can’t wrap my mind around that. I believe one day, in heaven, Jesus Himself will help me understand. But until that day, we continue here, to try to provide quality healthcare in Haiti, in Jesus’ name.